Glaucoma and stem cells
During a study to identify genes involved in the formation of glaucoma, researchers came up with a novel idea to take skin biopsies from participants with and without glaucoma. These skin cells were reprogrammed to regress to stem cells and then directed to develop into retinal cells. More than 200,000 individual cells were sequenced to generate ‘molecular signatures’. Both healthy and diseased individuals showed 312 genetic variants associated with the target retinal cells. Further analysis identified 97 genetic clusters linked to the damage caused by glaucoma. In this way, the researcher will be able to identify underlying mechanisms, possible causes, and risk factors involved in glaucoma.
Researchers in Maryland identified stem cells in the region of the optic nerve, which sends signals from the eye to the brain. These progenitor stem cells secrete growth factors and other factors for the stem cells to grow and replicate. Eventually, the research team found the stem cells could be guided to differentiate into various different types of neural cells. Thus, through further studies to identify the critical growth factors that these cells secrete, they may be potentially useful as a cocktail to slow the progression of glaucoma and other age-related vision disorders.
In a breakthrough in November of 2022, a research team from the Department of Ophthalmology, Indiana University School of Medicine, used induced pluripotent stem cells (iPSCs) from patients with and without glaucoma as well as engineered human embryonic stem cells with glaucoma mutations. Using stem cell differentiated retinal ganglion cells (hRGCs) of the optic nerve, electron microscopy, and metabolic analysis, they identified that retinal ganglion cells from glaucoma patients suffer mitochondrial deficiency with more metabolic burden on each mitochondrion. This leads to mitochondrial damage and degeneration (mitochondria are the tube-like structures in cells that produce adenosine triphosphate, the cell’s energy source).
However, the process could be reversed by increasing mitochondrial regeneration by means of a pharmacological agent. The team showed retinal ganglion cells are highly effective in destroying bad mitochondria, but at the same time producing more to maintain homeostasis.
The fact that retinal ganglion cells with glaucoma produce more adenosine triphosphate even with less mitochondria was a breakthrough. But when triggered to produce more mitochondria, the adenosine triphosphate production load was distributed among more mitochondrion which restored the organelle physiology. Whether these mechanisms protect the optic nerve will first be studied in animal models under injury before testing in humans to hopefully lead to new clinical interventions.
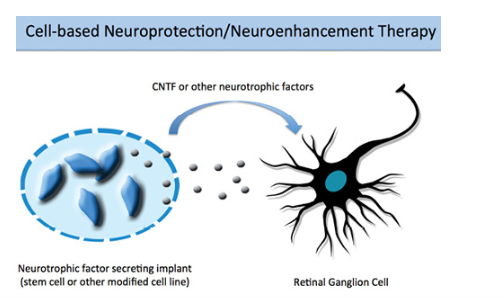
Image: Courtesy of BY DAVID I. GREEN, BS, AND YVONNE OU, MD. MAY/JUNE 2015 GLAUCOMA TODAY
Reviewing all the above discoveries; future stem cell transplantation might hold promise for possible treatment for glaucoma, with at least two different approaches; neuroprotection or replacement. Different transplanted stem cells, including retinal stem cells, neural stem cells and Mesenchymal Stem Cells (MSCs) have shown improved outcomes in glaucoma patients. The main mechanism of action seems to be due to neuroprotection linked to secreted factors and/or modulation of inflammation. However, scientists say, while stem cell transplant in glaucoma seems promising, further research is needed before it can become a standard treatment.
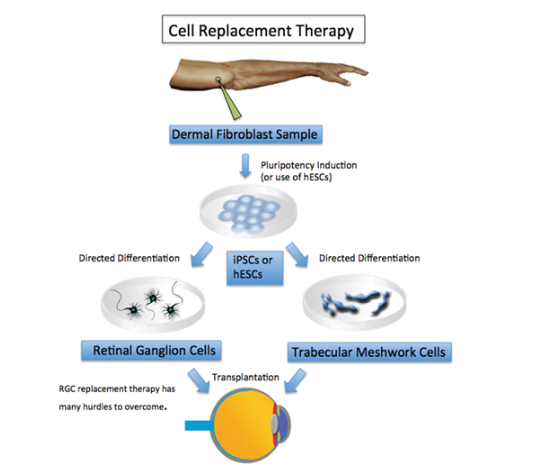
Image: Courtesy of BY DAVID I. GREEN, BS, AND YVONNE OU, MD. MAY/JUNE 2015 GLAUCOMA TODAY